CONCUSSION 101 GUIDE
Concussion Symptoms, Signs, Treatment, and Rehab
WHAT IS A CONCUSSION?
- Concussion is the most common type of traumatic brain injury.
- Every concussion is different; symptoms and recovery are different for everyone.
- Trained healthcare providers are the only ones who can diagnose and treat concussions.
- Post-concussion syndrome happens in 1 of 5 concussions.
- Not reporting a concussion puts you at risk for lasting damage.
- You can sleep after a concussion, as long as there aren't danger signs.
- One of the best ways to prepare for a concussion is to take a baseline test.
1. CONCUSSION BASICS
[Download Concussion 101 Guide]
WHAT IS A CONCUSSION?
A concussion is a head injury caused by moving forces such as a bump, blow, or jolt to the head, that results in a variety of symptoms and temporary changes in mental status, coordination, and balance.
Definitions are constantly updated based upon new research, but a concussion is a form of a traumatic brain injury. In fact, it’s the most common traumatic brain injury.
After a concussion, the symptoms that occur differ from patient to patient. These include headaches, dizziness, vision problems, trouble concentrating, feeling slowed down, repeated vomiting, sleep problems, and even irritability and sadness.
Symptoms may not even appear for days or weeks after the injury.
While sport-related concussions are the most commonly talked about, concussions can happen from falls, car accidents, or other traumatic events.
The good news is over 80% of patients diagnosed with a concussion usually get back to normal within three weeks, but some may have symptoms that last longer.
WHAT CAUSES A CONCUSSION?
Many people think that contact sports are the primary cause and that concussions are mostly a sports injury. Actually, according to the US Centers for Disease Control (CDC), falls are the main cause of concussions.
When a concussion occurs, there is an energy crisis in the brain. The impact of the brain against the skull can cause the brain to swell. It can even be life-threatening in rare cases.
Anyone is at risk for concussions. They occur frequently in sports (especially contact sports), but they can happen from falls, car accidents, and non-contact sports too.
Unfortunately, there isn’t a “cure-all” for the injury. There’s not a perfect way to prevent them, either.
An individual who has had a concussion can feel entirely back to normal with a short period of rest and proper treatment or rehabilitation.
WHAT IS A CONCUSSION PROTOCOL?
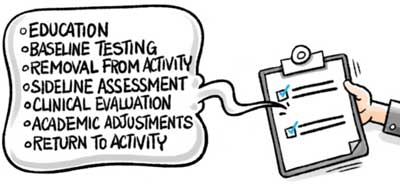
A concussion protocol is a standard for healthcare providers on how to diagnose and care for the injury. While protocols may differ depending on local laws or association policies, school/league concussion protocols should include at least:
- Pre-season education for parents and students;
- Comprehensive baseline testing procedures;
- Sideline evaluations after an injury;
- Clinical evaluation after an injury;
- Return to learn procedures;
- Return to play requirements.
WHAT IS POST-CONCUSSION SYNDROME?
Post-concussion syndrome happens when concussion symptoms stick around for weeks or months after the injury. It occurs in approximately only 20% of concussion cases.
Post-concussion syndrome can disrupt everyday activities, including school and social activities, and can feel like it will never improve.
When unrecognized or untreated, post-concussion syndrome can seriously affect daily life.
Your healthcare provider can help you get the proper treatment to improve your symptoms and return you to your everyday activities.

CAN YOU DIE FROM A CONCUSSION?
Unreported brain injuries can cause serious and lasting problems. However, research has shown that dying from a concussion is unlikely. Healthcare providers can help you recover and feel back to normal within 2 to 3 weeks most of the time.
HOW TO PREVENT CONCUSSIONS?
Unfortunately, there’s no easy answer in concussion prevention. Some parents think that keeping their children out of contact sports will prevent concussion.
However, a concussion can also be caused by non-contact sports, car accidents, and falls.
There are a variety of concussion “prevention” toys available on the marketplace. These devices claim to help prevent a concussion. However, there is little research available to support claims that a device can prevent a concussion.
The best plan is to get educated on concussion symptoms and take a baseline test. If your school or sports league does not offer baseline testing, you can take one yourself online, at home, in about 20 minutes.
After proper education, baseline testing is a great way to be prepared if you get a concussion.

WHAT IS BASELINE TESTING?
Baseline testing is a way of tracking your functioning at a healthy state. Baseline neurocognitive testing (like ImPACT and ImPACT Pediatric) measures how your brain functions when it’s not injured.
These tests measure reaction time, memory, and processing speed and give healthcare providers an accurate picture of your normal brain function. They can use that baseline test data to compare with post-injury data to determine the extent of your injury. They can also use this data to help decide when you’re back to normal cognitive functioning.
2. CONCUSSION SIGNS AND SYMPTOMS
[Download Concussion 101 Guide]
HOW TO TELL IF YOU HAVE A CONCUSSION?
Concussions can be tricky. Even trained healthcare providers may have a hard time diagnosing concussions because of its varying signs and symptoms. Concussions cannot be diagnosed with CT scans or MRIs.
Healthcare providers have to rely on clinical expertise and objective tools to help them diagnose and treat concussions. Look for a Concussion Care Provider if you’ve recently been hit in the head and experience any concussion symptoms. Keep in mind: most of the time concussions do not involve a loss of consciousness.

WHAT ARE CONCUSSION SYMPTOMS?
Concussion symptoms can vary drastically from person to person. Some show up right after the injury, like vomiting, dizziness, or headache. Some may show up days or weeks after the injury, like irritability, depression, or sleep problems. It is important to communicate regularly with your healthcare provider about any changes in your symptoms.
Research has shown that pre-existing risk factors may influence which concussion symptoms are experienced. For instance: an individual with a family history of migraine will likely experience migraine symptoms after head trauma. An individual with a lazy eye may experience vision problems after the head injury. Be sure that you talk about any medical conditions you have when you see a provider with a suspected concussion.
Again, you don’t need to lose consciousness to get a concussion. Check in with your healthcare provider if you experience any concussion symptoms and have recently experienced a blow to the head.
Concussion symptoms can include:
- Problems with concentration/memory
- Dizziness or lightheadedness
- Sensitivity to light or noise
- Change in sleep pattern
- Double or fuzzy vision
- Feeling foggy
- Headache
- Nausea
HOW LONG DO CONCUSSION SYMPTOMS LAST?
Concussion symptoms can last anywhere from a few days to weeks or months. This usually depends on whether or not the concussion is properly cared for. Post-concussion syndrome refers to lingering symptoms that last longer than the expected recovery time (about 3 weeks in adults, and up to a month in young children and adolescents).
Repeated concussions can cause symptoms to get much worse and can even cause life-threatening issues and long-term damage. It’s important that individuals speak up if they notice any concussion signs and a teammate acting out of character.
Concussion symptoms may sometimes look like other disorders, including depression or chronic migraines. If it’s happening to you or someone you know, recommend that they visit a healthcare provider to check for a concussion.
WHAT ARE THE SIGNS OF A CONCUSSION?
Concussion may have several signs visible to those familiar with an individual who’s recently experienced a blow to the head. There are many subtle signs that can point towards a concussion. Sometimes your teammates, coaches, or parents may be the ones to recognize these signs. Getting a concussion feels different for every person that experiences it. Symptoms differ drastically from person to person.
Signs of a concussion can include:
- Change in behavior
- Sleeping much more or less than usual
- Grades dropping for a student
- Increased anxiety
- Vomiting
- Dizziness
- Headaches
- Distractible
- Light or noise sensitivity
- Feeling worse in the afternoon compared to the morning
It's important to see a healthcare provider to check for a concussion if you notice these signs.
WHAT ARE THE CONCERNS WITH NOT REPORTING A CONCUSSION?
There are severe risks if you continue to participate in an activity after a head injury.
If you are not evaluated for a concussion by a trained healthcare provider, you may be at risk for second impact syndrome and post-concussion syndrome. It is important to tell someone if you have had a hit to the head or body and are feeling any symptoms that can be related to a concussion.
HOW DOES A CONCUSSION AFFECT SCHOOL PARTICIPATION?
If you have a concussion, your symptoms may limit your ability to participate normally in school. However, getting back to your regular schedule is important. Missing extra days of school can cause more harm than good. Your healthcare provider may recommend academic accommodations to get you back in school while you're recovering from a concussion. These can include class breaks, early dismissal between classes, reducing computer screen exposure, extra time to take tests, and more.
3. CONCUSSION DIAGNOSIS AND TREATMENT
[Download Concussion 101 Guide]
WHAT TO DO FOR A CONCUSSION?
Visit a trained healthcare provider if you think you have a concussion. This could be a physician or physician assistant, nurse practitioner, neuropsychologist, nurse, or an athletic trainer.
These individuals are trained to recognize concussions, and they can help you get the treatment you need. Most healthcare providers will recommend a brief period of rest followed by light activity that progresses back to full activity.
In some cases, your provider will recommend specific treatment or rehabilitation that targets the areas affected after a concussion.
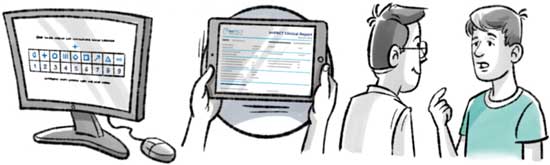
WHAT IS A CONCUSSION TEST?
A concussion test is a tool or device used to check a person’s level of functioning after a suspected concussion. There are several types of concussion tests, including neurocognitive, balance, vestibular ocular, motion sensors, and more. These tests do not diagnose concussion, but rather note deficits in function of areas known to be affected by a concussion.
Because concussion is such a hot topic, there are new devices being marketed regularly. While some tools or devices have been scientifically validated, others make claims that are not supported by science. There are many mobile apps that make untrue claims about their ability to detect a concussion.
Fortunately, there are some concussion tests that have been studied and found to be useful for assessing concussion. Healthcare providers have resources and research available to help them select validated tests. Most importantly, there is no one perfect concussion test. Healthcare providers need to use multiple sources to help them make concussion diagnosis and return to activity decisions.
Make sure your healthcare provider has the data they need to help you get better. Take a baseline test to ensure you have good comparison data after an injury.
HOW TO DIAGNOSE A CONCUSSION?
Healthcare providers use multiple tools and techniques to check for a concussion. There is no one perfect diagnostic tool. Clinicians rely on objective tools as well as clinical expertise and symptom reporting to help determine whether a patient has a concussion.
They may use any of the following tools to help make a concussion diagnosis:
- Clinical examination
- Neurocognitive testing (memory, reaction time, etc.)
- Balance testing
- Vestibular ocular testing
- Symptom inventories
HOW TO TREAT A CONCUSSION?
Concussion is treated differently depending on the symptoms a person has. Research has shown that active rehabilitation and actively targeting deficits a person experiencing is an excellent way to treat a concussion.
Similarly, someone who sustains a concussion for the first time will be treated differently than someone who has had repeated concussions. Common concussion treatments include vision therapy, vestibular therapy, and exertion therapy.
HOW LONG DOES A CONCUSSION LAST?
Concussion recovery times vary depending on the severity of the head injury and how it is treated. If properly treated, most patients recover from concussions in 2 to 3 weeks.
Some people think that the best way to treat a concussion is to rest and stay away from activity. However, research has shown that this is not the case. In fact, patients who participate in active rehab are more likely to get back to school, work, and activity more quickly.
Trained healthcare providers recommend a brief period of rest followed by increasing physical activity. For patients who experience post-concussion syndrome, recovery can take longer, up to a few months if not treated properly.

WHAT ARE RETURN TO PLAY CRITERIA?
If a healthcare professional removes you from activity for a suspected concussion, they will conduct a sideline assessment to determine if you have a concussion. If you're diagnosed with a concussion, you will not be allowed to return to play that day.
Once your brain is healing and you're showing progress, you'll go through a gradual return to activity process. This process, supervised by a healthcare provider, includes the following steps:
- Symptom-limited activity
- Light aerobic exercise
- Sport-specific exercise
- Non-contact training drills
- Full contact practice
- Return to activity
In order to return to play, you'll need to be:
- Symptom-free:
- At rest
- With cognitive exertion
- With physical exertion
- Without any medications (if introduced during recovery)
- Within normal limits on:
- Balance (BESS)
- Vestibular Ocular Screening (VOMS)
- Back to (or better than) baseline on neurocognitive testing scores
Download a Return to Activity Checklist.
CONCUSSION AND SLEEP: WHAT PRECAUTIONS SHOULD BE TAKEN?
It’s a common myth that you shouldn’t sleep after a concussion. In fact, sleep can help your brain get the rest it needs after a concussion, especially in the first 24 hours. As long as you don't present danger signs, you can sleep. Get the truth about other common concussion myths.
Danger signs can include dilated pupils, slurred speech, worsening headaches, confusion, or loss of consciousness. If they do show some of these signs, you may want to go to the emergency department for a physical examination.


